Feeding is very much a normal part of motherhood. You assume you will nurture your child, and that it will be a fulfilling and rewarding experience. When you face challenges, not only can it be completely frustrating and demoralising, it can come to dominate your life. Feeding issues are extremely common with babies suffering from Edwards Syndrome. Many lack the ability to co-ordinate sucking, swallowing and breathing all at the same time.
Breast feeding
My Mummy had initially hoped to breast feed me. Once my condition was diagnosed she was even more adamant that I should have breast milk to help build up my immune system. However I was far too weak to even attempt this. Instead she expressed every 3 hours in line with my feeds.
Milk from a syringe, bottle & drip
Whilst I remained in hospital care, my feeding had been a mix of taking tiny quantities of milk from a syringe, occasionally from a bottle and in the very early days via a drip. Upon discharge from hospital, my parents were offered to have a naso-gastric tube fitted to help with feeds. Based on all the knowledge that had been shared with them, this seemed the best step forward.
Naso-gastric feeding tube
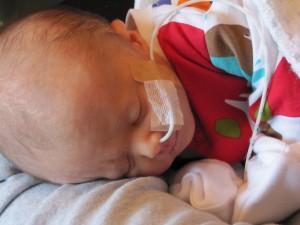 The thought of feeding a baby via a naso-gastric tube might seem awful at first. However, despite the fact I didn’t like it, it was relatively easy for Mummy and Daddy to use. The tube was inserted via my nose down into my stomach, with some tubing and a bung/stopper secured onto my face. Look here I am with mine:
The thought of feeding a baby via a naso-gastric tube might seem awful at first. However, despite the fact I didn’t like it, it was relatively easy for Mummy and Daddy to use. The tube was inserted via my nose down into my stomach, with some tubing and a bung/stopper secured onto my face. Look here I am with mine:
In the main apart from mild discomfort whilst it is fitted, most children/babies take well to the tubes. It is unclear why I didn’t…but I came to hate it in the end, and I let everyone know too!!!
Using a feeding tube
Once fitted, on each feed there are a sequence of steps that need to be taken. The first is to make sure the baby is in a comfortable position. Usually on their side helps. Then you attach a syringe to the feeding tube, and attempt to draw back any fluid that you can. This is done, as you need to test to make sure the tube is actually in the stomach. Any fluid you draw back you test on a piece of litmus paper, and if it turns red this is fine, as the stomach juices are acidic. If it doesn’t, it means the tube is not inserted correctly (and could be in the lungs) and it should be re-fitted.
Once you know it is OK to go ahead, you fill a separate syringe with milk and attach it to the bung. You should keep the syringe up slightly to ease the flow of milk down into the tube, but make sure it doesn’t go down too quickly.
Once all the milk has been used up, you just need to remove the syringe, and attach one final syringe with a small amount of sterile water in it. This is used to flush the tube and to make sure that it doesn’t get clogged up. That is it!!!
Bottle feeding
Mummy and Daddy had always allowed me to take a little milk from a syringe orally before each of my NG tube feeds. They wanted me to taste things as much as I could, but also they didn’t want my throat and mouth getting too dry.
As a result, it was noticed that I had quite a good suck when I was doing this. So much so that my friends at the hospice helped to get me feeding entirely from a bottle. My tube was quickly removed, and everyone seemed so much happier feeding me this way. It also meant I didn’t have the tube across my face which was great for pictures, and stopped people asking questions when they met me.
My parents experimented with lots of different shaped teats, and eventually it looked as though the best solution was a NUK bottle and teat.
All went well to begin with, I took all of my feeds without a problem. However, over a few weeks it started to get harder and harder for me. I lacked the energy and co-ordination to suck, swallow and breathe and I started taking less and less milk, and taking longer and longer to consume whatever amounts I would take.
One final attempt at bottle feeding was with something called a Haberman Feeder. Milk is released into a long teat, and parents are able to help by squeezing the teat to help with the flow of milk. It is quite commonly used for babies with Cleft Palates. The bottle also reduces Colic. Despite several attempts however, this did not seem to work for me.
Syringe feeding
As I refused to have the tube re-fitted, eventually my parents had to resort to Syringe feeding me. In terms of the process, it is relatively simple. A syringe is filled with milk, and the milk is drip fed into my mouth. I don’t know what was wrong with my feeding though, no-one was able to find out, but I would scream all the time. Syringe feeding would take longer due to the small quantities I was taking in one go, and Mummy hated it, because I was so unhappy. But in the end it was the only way to feed me.
Oro-gastric feeding tube/Stomach feeding tube (Gastrostomy tube)
Although I never had either of these, it is possible to have an Oro-gastric tube rather than a naso- gastric tube. (I think I would have probably have pulled this out just as easily had I had it fitted).
The gastrostomy tube, has to be inserted via a minor operation, and so it usually used by children who are a little older/larger, and who are strong enough to take an anaesthetic.
Frequency & Quantity of feeds
When I first came home from hospital I was on a 3 hourly feed cycle. I was taking around 40-45mls with each feed. The 3 hourly cycle initially seemed to work like clockwork. I took my milk easily, and rarely cried between feeds.
As I got a little older, and I enjoyed feeding less and less, my parents experimented with all sorts of feeding patterns. This included demand feeding, feeding me smaller quantities more frequently (every 2 hours for example). Demand feeding didn’t seem to work that well, as I rarely cried for food, and on occasions was prepared to go very long periods without a feed (10-12 hours). Very little seemed to make any difference to how well I fed, or whether I kept my feed down or not.
Ultimately the best pattern, seemed to be the one we started with, which was about every 3 hours.
The quantity of milk I took didn’t really alter that much, as I gained such little weight. My maximum feed was about 400mls a day on expressed milk, although when I moved to formula this decreased as the milk was more calorific.
Milk & food
I started on milk Mummy was expressing for me. I had no problem with this, although my weight gain was only slight. As I got a bit more difficult to feed, and was bringing my milk back up, Mummy was struggling to keep up with sufficient production of milk.
She could take medicine to improve her production, but as it also acted as a diuretic, which might pass to me, she was advised not to.
In the end Mummy conceded defeat, and with advice from a Dietician at the Children’s Hospital, I was moved onto a more calorific formula milk called Infatrini. This Milk was on prescription, so Mummy had to regularly call the Dietician with my weight gains, to assess how the feeding was going, and whether more milk should be prescribed.
Initially, I took the milk well, but eventually, as before I just stopped enjoying feeds. Poor Mummy tried everything. She even put Crusha in my formula once to see if this might help, but it didn’t. She also started to wean me. I don’t think she ever had any hope that I might feed properly, but she did want me to experience different tastes, and if it helped break up the nasty feed experiences, she thought it was worth trying. So I got to taste things like Carrot, Parsnip, Baby Rice, Sweet Potato, but my absolute favourites were the sweet things like Apple, Pear and especially Banana. Mummy made sure these foods were in addition to my milk though and not as a substitute.
The final thing Mummy tried, with the help of the hospice was something called ‘Thick and Easy’. It is basically a thickener. There was a thought that perhaps the milk was too runny, and that my discomfort might be caused by me panicking A thicker milk can make breathing and swallowing easier. I took my feeds well when this was added to my milk, but sadly it was only tested on my final few days, so there is no lasting proof of whether it would have worked long term or not. However, I enjoyed my final few feeds, and for that Mummy is very grateful.
Colic, constipation & reflux
I had all of these at one stage or another, and all of which helped me enjoy my feeds even less.
Initially with the tube fitted, I had very few problems, but as we moved onto Bottle feeding so the Colic would kick in. Having barely screamed at all those first few weeks, suddenly I found my lungs, and I let my parents know I was uncomfortable. They tried using Infacol, but it seemed to make little difference.
Eventually the Colic did ease but it was replaced by Constipation and Reflux. The constipation started when I was moved onto formula milk. Although my stools were soft, I was going less and less frequently, and I seemed to be in discomfort. Mummy took me to see the GP and I was given something called Lactulose. I really liked this as it was nice and sweet, and I would smack my lips whenever I drank it. It helped too 
On a trip to A & E, and having met a nice Doctor as well as My Dietician, it was also agreed to put me on some reflux medication. Mummy had to write it all down, as she didn’t want to forget all the things I had to take and when. On top of the lactulose, Mummy also had to mix Baby Gaviscon into my formula milk, and also dilute an Omeprazole tablet, which I was given a small quantity of once a day.
Speech therapy/Community Dietician
My parents wanted me to see a Speech Therapist to see if they could give any advice on my continual feeding issues (they can watch you feed, and recommend different bottles, teats etc). Sadly, the appointment came too late for me, and we were unable to find out if this would have provided the ‘solution’.
My parents also wanted me to see a Community Dietician. We were pretty housebound most of the time, and getting to the Children’s Hospital to see the Dietician based there was difficult. We weren’t sure if there were other milks that I should have maybe tried, or if there were any other options. However, we were told that because I no longer had the tube fitted, I didn’t match the criteria for being referred to a Community Dietician. It seemed so illogical as my feeding was in a much worse state than if I had been able to take the tube.
